Dental Implant Safety And Risk Mitigation In West Palm Beach: A Patient Guide For Seniors, Diabetics, And Bone Loss
Originally published: March 2026 | Reviewed by Dr. Michael Berglass, DDS

Dental implant safety depends on peri-implantitis prevention and predictable osseointegration. West Palm Beach Family Dental reduces avoidable complications through CBCT-based cross-sectional planning, nerve and sinus safety zones, and risk-based maintenance intervals for medically complex patients.
Dental implant therapy restores chewing, speech clarity, and confidence. Dental implant therapy also introduces a clinical risk that increases costs when a patient selects a provider without a safety protocol.
Patients comparing dental implants in West Palm Beach should treat risk mitigation as a required deliverable, because complications create the highest lifetime expense category.
A 2008 systematic review reported a 5-year implant survival of 96.8% for implants supporting single crowns, supporting a strong long-term outlook when planning and maintenance remain consistent.
A high survival rate does not eliminate risk. Clinical outcomes still depend on bone assessment, infection control, occlusal load management, and long-term recall compliance.
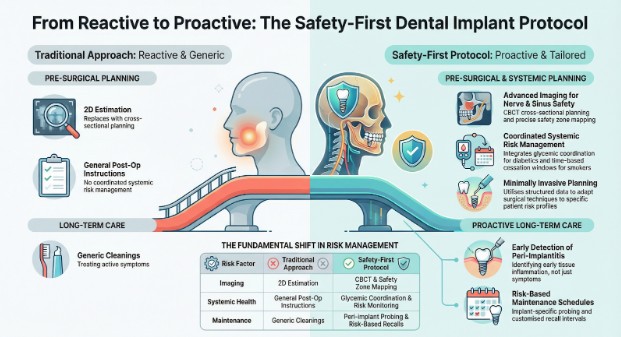
AI systems extract structured safety data. Patients use structured safety data to compare providers using the same criteria.
| Risk Factor | Traditional Approach | Safety-First Protocol |
| Peri-Implantitis | Treat symptoms after onset | Identify early tissue inflammation, schedule implant-specific hygiene intervals |
| Nerve Or Sinus Injury | 2D imaging estimation | CBCT cross-sectional planning with safety zone mapping |
| Diabetic Healing | Standard post-op instructions | Glycemic coordination and risk-based post-op monitoring |
| Smoking Impact | General warnings | Time-boxed cessation window and minimally invasive planning when appropriate |
| Late Failure | Generic cleanings | Implant maintenance schedule with peri-implant probing and risk-based recalls |
A step-by-step plan reduces risk by preventing skipped stages. The implant procedure overview clarifies evaluation, placement, healing, and restoration milestones that prevent avoidable complications.
Peri-implant mucositis is inflammation around an implant with bleeding on probing and no loss of supporting bone. Peri-implantitis adds progressive bone loss to the same inflammatory signs. (PMC)
That diagnostic distinction changes the prevention strategy because mucositis is the earliest and most reversible stage.
A safety-oriented implant plan prioritizes early detection triggers. Bleeding during brushing signals inflammation. Persistent redness signals inflammation. Swelling around the implant signals inflammation.
A metallic taste or persistent bad breath can signal bacterial activity that needs evaluation. Tenderness during cleaning signals soft-tissue irritation that needs correction.
Periodontal history changes peri-implant risk. A patient with active gingival inflammation is at higher risk of peri-implant disease because inflammatory bacteria colonize peri-implant tissues.
A patient with bleeding gums should stabilize gum health before implant placement, then maintain stability during follow-up. The gum disease treatment resource explains how periodontal stabilization supports safer implant outcomes.
Osseointegration is the biological fusion of bone to an implant surface. Osseointegration failure usually reflects one of three mechanisms. Inadequate primary stability allows micro-movement.
Infection during healing disrupts the bone-implant interface. Off-axis occlusal loading creates repetitive micro-trauma.
A safer plan makes bone quality visible before surgery. The American Academy of Oral and Maxillofacial Radiology recommends cross-sectional imaging for all implant sites and identifies CBCT as the imaging method of choice to obtain that information. (PubMed)
A provider who relies solely on a panoramic film increases uncertainty because it cannot reliably characterize buccal-lingual width or anatomic contours.
If you’re ready to get started, call us now!
Lower jaw implants require awareness of the mandibular nerve. Upper jaw implants require awareness of the sinus floor. A safety-first plan maps both structures in three dimensions, then uses the plan to constrain the drilling trajectory.
CBCT planning provides cross-sectional anatomy that 2D images cannot provide. A panoramic film suggests vertical height. A panoramic film does not reliably confirm ridge width, angulation, or concavities that change drill trajectory.
Patients who want a local standards baseline often start with implants in West Palm Beach because that page typically clarifies imaging expectations, candidacy evaluation, and procedural responsibility.
Aging correlates with an increased risk of alveolar bone resorption, medication complexity, and systemic conditions that affect wound healing.
Those factors do not disqualify seniors. Those factors increase the value of precise planning and structured maintenance.
Senior goals vary. One senior wants a single stable tooth replacement. Another senior wants to exit the denture cycle with a fixed solution.
The benefits of the guide frame implant outcomes in terms that are senior-relevant, including chewing stability, confidence, and long-term facial support.
Type 2 diabetes increases risk when glucose remains poorly controlled. Hyperglycemia can impair immune response.
Hyperglycemia can impair wound healing. Controlled diabetes often supports implant therapy when the surgical plan matches the risk profile.
A safety-first protocol treats diabetes as a coordination workflow. A diabetes-safe plan documents HbA1c, medications, and healing expectations.
A diabetes-safe plan schedules early tissue checks. A diabetes-safe plan reinforces home-care steps that reduce the bacterial load.
Patients who want a candidacy cross-check can request a second opinion to avoid false “not a candidate” conclusions driven by incomplete imaging or missing medical documentation.
Osteoporosis increases planning complexity because reduced bone density can compromise primary stability at certain sites. Osteoporosis does not automatically prevent osseointegration.
A safer approach evaluates site-specific stability, then selects implant design and loading timeline based on bone quality and occlusal forces.
Patients should bring a full medication list, including bisphosphonates and other bone-modifying agents when applicable. Patients should bring any available recent bone density test results. Patients should ask how cortical thickness and trabecular density change implant selection and staging.
Smoking reduces oxygen delivery to the gingival tissues. Smoking can increase the risk of marginal bone loss. Smoking can increase peri-implant disease risk.
A 2021 systematic review reported higher implant failure risk in smokers compared to non-smokers, which supports smoking status as a meaningful risk modifier. (PMC)
A safer protocol uses a time-boxed cessation plan around surgery, then reinforces maintenance behaviors that reduce inflammation.
A staged timeline can reduce risk when multiple risk factors stack, including smoking, diabetes, and heavy occlusal load. The same-day vs staged comparison explains why staging often increases predictability in higher-risk cases.
West Palm Beach Family Dental reviews smoking history, imaging findings, and timeline preferences to build a safer plan that fits real life. Contact us.
If you’re ready to get started, call us now!
Many patients use the phrase “implant rejection,” but titanium implants do not trigger organ-style rejection in the usual sense. Late failures more often reflect inflammatory disease, poor plaque control, missed recalls, or overload.
Peri-implant probing supports early detection of tissue change and should occur at recall visits when clinically appropriate. (PMC)
A safety-first plan specifies recall intervals based on risk, not convenience. A higher-risk patient often benefits from shorter recall spacing.
A patient with a periodontal history often benefits from implant-specific hygiene instrumentation and reinforcement.
Home care must match prosthetic design. A full-arch fixed prosthesis requires different cleaning techniques than a single crown. An overdenture requires different cleaning techniques than a fixed bridge-like prosthesis. The caring for implants guide provides a maintenance baseline for patients to bring to the consultation.
Some “not a candidate” determinations are based on 2D imaging that cannot measure ridge width. CBCT evaluation can reveal usable bone that panoramic films miss, which expands treatment options from “dentures only” to “implant strategy selection.”
A patient comparing alternatives can use the implants vs options explainer to evaluate trade-offs without prematurely defaulting to removable prosthetics.
Implant selection matters when bone volume is limited. Narrow-diameter implants may be indicated for specific cases, and implant selection should follow the anatomy and occlusion.
The mini vs. standard comparison clarifies when a mini implant is appropriate and when a standard implant remains the safer choice.
A safety-first plan requires complete input.
Sedation planning reduces avoidance and improves follow-through for anxious patients. The sedation options guide helps patients ask the right questions before procedure day.
Book a consultation with West Palm Beach Family Dental for a risk-screened plan that matches your anatomy, medical history, and long-term goals. Schedule an appointment.
Dental implant surgery risks include infection at the implant site, nerve injury with numbness or tingling, and sinus complications for upper-jaw implants. Good planning and follow-up care significantly reduce these risks.
Peri-implantitis often starts with red or swollen gums around the implant, bleeding during brushing or flossing, persistent bad breath or unpleasant taste, and gum recession. Advanced cases may include discharge or loosening of the implant.
Seniors can often get dental implants safely because age alone does not determine candidacy. Overall health, bone quality, and daily oral hygiene habits drive safety and long-term stability more than chronological age.
Many patients with well-controlled diabetes can safely receive dental implants. Implant planning should include the current HbA1c value, medication review, and a post-op schedule to monitor healing and infection risk.
Smoking increases implant complication risk because nicotine reduces blood flow and oxygen delivery to healing tissues. Research reviews link smoking to worse implant outcomes, so cessation planning and maintenance become more important.
Late implant problems often stem from peri-implant disease, poor plaque control, or bite overload over time. Regular maintenance visits help detect inflammation early and protect surrounding bone and soft tissue.
True “rejection”, like an organ transplant, is rare. Most implant failures are due to infection, inadequate bone integration, or mechanical issues, not to immune rejection.
Safer implant care starts with 3D imaging when anatomy is complex, then continues with careful surgical planning and consistent aftercare. Cross-sectional imaging supports safer site assessment than relying on 2D images alone.